At the recent QMP aesthetic surgery symposium in Chicago, our own Dr. Simeon Wall Jr. participated in a “point-counterpoint” panel discussion with Dr. Fabio Nahas. The panel covered hot topics in liposuction and abdominoplasty, and was moderated by Dr. James Grotting. Dr. Wall Jr. was among a select group of world-renowned plastic surgery faculty to lecture on a wide range of topics in cosmetic plastic surgery at the symposium.
Point and Counterpoint: Practical and Clinical Aspects of Body Contouring and Abdominoplasty
Moderator: James C. GrottingMD FACS
Discussants: Simeon Wall Jr. MD; Fabio Nahas MD PhD
Moderator, Dr. Grotting: The discussants in this “Point and Counterpoint” article are two of the world’s experts in abdominoplasty and body contouring: Dr. Simeon Wall Jr., from Shreveport, Louisiana, and Dr. Fabio Nahas, from Sao Paulo, Brazil.
I would like to pose some questions to our experts. The first concerns the use of drains in abdominoplasty, or the use of drains with liposuction alone. Dr. Wall, what do you think about the use of drains in liposuction?
Dr. Wall: I almost always perform circumferential trunk liposuction, and I put in a single drain threaded across the lower abdomen; I do not routinely drain anywhere else, but I do leave all of my incisions open to drain. Over the first 2 to 4 days, there is a lot of drainage coming out of the open incisions, and I think it dramatically reduces the bruising, if it does not eliminate it, and it helps eliminate a lot of the early swelling. So, I do use a drain in the abdomen, and pretty much not anywhere else.
Moderator: Is there something unique about the abdomen in terms of producing more fluid than some of the other areas that we routinely contour?
Dr. Wall: Well, the circumferential trunk is probably the biggest area with the greatest potential for fluid accumulation, and I do think it is important to minimize the potential for a seroma. I do not think it is necessary to routinely thread a drain all the way around the back, because the drains I use are the extra long 15 Fr round Blake drains. The drain goes in one side of the abdomen and reaches across the front to the other side, and most of the fluid is handled by that single drain. The other areas we routinely contour are probably not large enough to accumulate fluid requiring a drain, especially because I leave all those incisions open.
Moderator: Dr. Nahas, what do you think about the use of drains in liposuction?
Dr. Nahas: I want to separate liposuction from abdominoplasty to answer that. During abdominoplasty, when I do the stitches with quilting sutures, I use a Penrose drain, because there is very little space for blood collection when I use that technique. I usually place these drains for 24 hours. When I do not use quilting sutures, I use a continuous suction drain that I set at a flow of about 40 ml. I remove the drain around postoperative day 4 to 6. I do not use any drain after liposuction; I just suture the incisions. I think that, with this method, patients do not feel the fluid draining and do not get wet, and so it is more comfortable for them.
Moderator: My next question is this: Does retained fluid after liposuction alter the final result? Obviously, Dr. Nahas thinks that the fluid is just absorbed over time, and Dr. Wall thinks that getting the fluid out may contribute to an improved postoperative result. Is that true?
Dr. Wall: Yes, absolutely. I looked at this when I used to close the incisions and leave multiple drains in. There can be hundreds of milliliters of fluid coming out of the circumferential trunk in the first day or two alone, which is several hundred milliliters less than would otherwise have to be absorbed or become a seroma. I think that all that fluid can do is sit inside the body and hinder the final result, and the tissues can start to stick together a lot easier by eliminating the fluid, not to mention that there is almost no bruising this way. It is rare for me to see any bruising when I allow all the fluid to escape through the open incisions.
Moderator: Dr. Nahas, what do you think about the retained fluid?
Dr. Nahas: I do not think exactly like Dr. Wall does, perhaps because I perform the operation with the patient in the supine position, and then I turn the patient prone. This means that when I am working on the anterior abdominal wall, the back of the patient is pressed against the operating table. When I turn the patient downward, I press the area that I have just aspirated. I think it is because of this that I do not see a lot of edema and fluid collection in the anterior and posterior abdominal wall. However, I do see some collections on the flank that, in some cases, can get a little bit stiff after the surgery. However, the reason I do not leave any incisions open is that the collection will go out and will fill the subcutaneous area or the liposuction area, and, by leaving it open, some fluid and blood may be lost.
Moderator: I would like to get both of your opinions on the use of pressure garments, and how these garments affect fluid collection following liposuction.
Dr. Wall: I routinely use compression garments for procedures on all areas of the body and the face. I think that compression is very important. I have tried immediate compression for a long period of time, all the way down to no compression, and I always go back to using compression. I think that it controls the area a lot better, and I find that, in addition to leaving the incisions open, it helps to greatly reduce immediate swelling. Patients are a lot more comfortable with a compression garment than without one. I would love to not have to use compression on patients, but I do think that it is necessary.
Dr. Nahas: I still use compression garments, but I am reevaluating. The reason I am rethinking this subject is that I am doing a study on the pressure of the femoral vein, and there is a big increase when you put those garments on. I have only preliminary results so far, but when I have the final results, I will either change the type of garments I am using, or I will discontinue using them.
Dr. Wall: I think that is a great point, and that is something we all worry about–increasing the chance of a deep vein thrombosis or a pulmonary embolism by using compression garments, and decreasing pelvic or lower extremity blood flow. One thing I have moved toward over the last several years is to use looser compression garments. A garment that is too tight can crease, which can fold the skin, especially when a patient bends over, and this can result in a permanent contour deformity. Ideally, I want to use just enough compression to keep the skin smooth and flat. To clarify, I do not use a compression garment initially after abdominoplasty. Instead, I use a very loose abdominal binder for the first 72 hours, so that pelvic blood flow is not decreased. Then the patient is instructed to wear a compression garment that would normally be considered about a size too large.
Dr. Nahas: That is probably a good idea, because the study I mentioned measures the femoral vein pressure before surgery, with and without the garment, and after surgery, with and without the garment. The next study that we are going to do will compare two different types of garments: one that is placed over the abdomen with a Velcro binding and another one that is much more comfortable for the patient–the kind used by plastic surgeons. We have to think about the increasing pressure, because there are a lot of factors that increase pressure in an abdominoplasty, which means decreasing the flow in the femoral vein. One of the factors is the number of vessels cut, which can cause blood to be held in the upper part of the body. Then there is the plication, which also exerts pressure in the caval vein. Then there is the position of the patient’s body and the belt garment. All these pressures together can decrease flow in the femoral vein.
Moderator: Do you put abdominoplasty patients into garments immediately?
Dr. Nahas: Yes. That is what I currently do, but I am reconsidering it. As soon as I have the data from our study analyzed, I will be able to comment on that more properly, and perhaps I will change the way I use garments.
Moderator: Dr. Nahas mentioned the use of quilting sutures. Dr. Wall, how do you feel about this kind of suture in abdominoplasty?
Dr. Wall: I think Dr. Nahas has eloquently described the difference between Baroudi-type quilting sutures and the progressive-tension sutures described by Pollock and Pollock.1 I started using progressive-tension sutures about 4 years ago, and they have resulted in a dramatic difference in seroma formation. I have tried different maneuvers over the years to decrease seroma occurrence, but once I started using progressive-tension sutures, the incidence of seroma dropped to where it is very rare now. It also really decreases tension on the flap closure, which ultimately results in better scars. Patients have more mobility, there is less shear, there seems to be less pain, and patients even recover a little faster. So I firmly believe in progressive-tension sutures; I think they accomplish a lot of things, and they are a significant advance in abdominoplasty surgery.
Moderator: Can both of you briefly describe, technically, how you place these sutures? What does your assistant do as the sutures are being placed?
Dr. Nahas: The needle should not pass very superficially to the skin–instead it should be passed on Scarpa’s fascia. The assistant then advances the flap as much as possible, and I attach the flap toward the fascia. Stitches are placed every 2 cm, because, if I put in very few stitches, there are areas in between the stitches where seromas can collect, and I may fail to clinically diagnose them. If that happens, contractures and deformities may develop in the flap. Therefore I place a lot of these stitches at the end of the surgery.
Dr. Wall: I do not use as many progressive-tension sutures as Dr. Nahas does. I use between six and nine stitches under the body of the flap, and then the Scarpa’s fascia closure is sutured to the abdominal fascia. But unlike Dr. Nahas, I pass the needle in the abdominal fascia at the level where I want the suture, and then, with the opposite hand, I advance the flap on the fascia as far as I can and put the maximal amount of tension that I want to see on the flap. When the abdominal fascia and the flap meet, I pass the needle through Scarpa’s fascia on the flap and then tie that down. I place from three to five sutures at the level of the umbilicus or above, and it is particularly important to prevent any dead space formation in the midline. I use sutures sparsely below the umbilicus, because I suture the flap to the fascia at the level of the closure.
Moderator: Do you also use drains in abdominoplasty, and how long do you leave them in?
Dr. Wall: That might be one reason that I do not use as many progressive-tension sutures, because I still put two 15 Fr round Blake drains in the abdominoplasty, exiting from the mons area and extending out laterally in the lower abdominal space. I leave those drains in until there is less than 25 ml of output each day, which is anywhere from 3 to 8 days. I think the average is about 5 days.
Moderator: Do you think it is safe to perform an abdominoplasty on patients who smoke?
Dr. Nahas: I do operate on patients who smoke. However, I try to persuade them to quit smoking for at least 15 days before the operation. If they do not stop smoking, I share with them all the potential consequences of necrosis. I show them pictures, and I do the operation, knowing that they have an increased risk of developing necrosis. However, I will not perform liposuction of the flap, and I will not remove any underlying tissue or fascia–I will not perform a lipectomy. That is important, because the more procedures done on a flap in a patient who smokes, the more likely complications are.
Dr. Wall: We do not operate on smokers as a rule in our practice, and if we have anyone who is undergoing a larger procedure, such as an abdominoplasty, a mastopexy, breast reduction, face lift, or any type of flap, we have them stop smoking for at least 4 weeks before surgery. We also perform a nicotine test on them at their preoperative visit, which is usually 4 to 10 days before their surgery. If the result of the nicotine test is positive, we will not do the surgery. For us, it is not worth risking a bad complication that is entirely preventable. I have always felt very strongly about not operating on a smoker, and if the surgery is important enough for them to stop smoking, then they will probably be compliant otherwise, as well. If they cannot stop smoking, that is probably a bad indicator all around.
Moderator: What do you advise women who request abdominoplasty before having children?
Dr. Nahas: If a patient has never had a child, I advise her not to undergo an abdominoplasty. I explain that if she undergoes the operation and then gets pregnant, I may not be able to provide the best treatment. However, there can be exceptions; I will give you an example. One of my patients was an 18-year-old model who had gotten pregnant when she was 16; she was a beautiful girl, but her career had stopped because she had a lot of striae. Her mother came with her, and they asked me to proceed with the operation, because otherwise her career would end. I tried to convince them otherwise, and I asked them to think over what I had told them regarding the potential consequences of the procedure for her. They returned and asked me to do the operation, so I performed the abdominoplasty. Later, I was very satisfied when I saw this patient on TV doing a fashion show, proving that she could go back to modeling again. It is very important to see a patient not as a statistic–18 years old, with or without children–but as a whole person. I had one patient who had a child 2 years after an abdominoplasty, and she did not have a recurrent soft diastasis, and she regained her figure through a workout regimen. She had the one child and could have more.
Dr. Wall: I agree with Dr. Nahas that these cases need to be looked at individually, but unfortunately, it is becoming more common for me to see younger women who have not yet had children but have a full abdominal pannus and request abdominoplasty. Usually these are massive-weight-loss patients, from gastric bypass or from diet and exercise, but these cases are always tough, and, like Dr. Nahas, I try to discourage these patients, especially those who are not done having children. They should wait, if they can. For example, one of my patients was a 17-year-old girl who had lost 180 pounds from diet and exercise. She was single and wanted to wear normal clothes and to date. She had a very large pannus and a very ptotic mons, which is a very abnormal body shape for someone so young. In cases such as this I do perform the abdominoplasty, but I also do not to perform any plication of the abdominal wall unless it is absolutely necessary. In such cases, I can usually produce a very reasonable result through skin contouring and liposuction without having to worry about a future pregnancy harming the patient because of abdominal wall plication. On rare occasions when I do have to perform some plication, I always use an absorbable suture, and I definitely do not overtighten.
Moderator: During surgery, if you find that a patient has rectus muscles that are apposed to each other, will these patients still benefit from plication if there is no indication of rectus diastasis?
Dr. Nahas: Such patients usually have had pregnancies, or they were formerly obese, so their abdominal wall distention is very large. I do not remember a single case in which I decided not to do the plication, except in patients who may have children later. I have had four or five cases of younger patients, about 18 years old, who had undergone gastroplasties, and I did not do the plication because I thought that they might have children in the future. However, they all ended up with some diastasis because of the increased pressure from fat inside the abdominal cavity.
Dr. Wall: I agree. I do not have much to add to that. It is not common to decide intraoperatively not to do a plication when I thought preoperatively that I would.
Moderator: My final question is this: Is there an age limit for abdominoplasty beyond which you feel it is not safe to perform it?
Dr. Nahas: I have performed abdominoplasties in patients older than 70 years. I do not think I would perform the procedure in a patient who is 80 years old or older. I do not believe there is really an age limit, but I think the sensibility of the surgeon counts in deciding which patients should be operated on. Recently I had an older patient with a colostomy who wanted a breast lift. She had had cancer, and she came with her husband, who told me that he wanted his wife to be happy about her breasts. I performed the breast lift, and 2 or 3 years afterward the patient came back and told me that she was very satisfied with the results I had achieved, but that she would like to have firmer breasts. This patient had a pulmonary embolism from her previous colectomy surgery, so I reminded her that she was 72 years old, and that I would have to change the prostheses when she was 82. But she and her husband convinced me that they had a very active sex life, and they wanted to go ahead with the procedure. So I placed the prostheses for her, even though I do not know what will happen when they need to be replaced. They are very satisfied with the outcome, and I still see them, so I think I did the right thing.
Dr. Wall: I do not have a set age limit for performing abdominoplasty, although I do think that patients older than 65 have a more difficult time with recovery–but there are always exceptions. For patients who are 65 or older, I use a more extensive workup to clear them; I make certain that an internist clears them very extensively, and I assess them using pretty tight BMI standards. Older than age 70, I start to have a hard time with this, but again, I do not have a firm rule.
Moderator: Thank you both for your insights.
Patient Examples From Dr. Wall

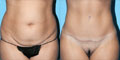
This 37-year-old mother of 16-year-old twins presented with complaints of loose, sagging trunk skin, and loss of waist and buttock definition. Abdominoplasty and liposuction of the circumferential trunk were performed. The liposuction aspirate was 2.5 L, and the pannus weighed 1320 g (Fig. 1). She is shown preoperatively and at 8 months postoperatively (Fig 2). Notice the overall truncal contour improvement, including an improvement in the shape of her back and buttocks. The combination of excising all of the sub-Scarpa’s fat in the entire flap and aggressive liposuction of the remaining circumferential trunk gives a more defined and sculpted appearance of the underlying abdominal musculature.
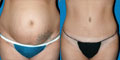
This 26-year-old mother of two presented with complaints of asymmetrical and ptotic breasts, severe abdominal rectus diastasis, and loss of truncal contour. She is shown preoperatively and 8 months after vertical mastopexy and abdominoplasty with liposuction of the circumferential trunk. Nineteen grams of tissue were removed from the right breast and 152 g were removed from the left. The liposuction aspirate was 3.7 L, and the pannus weighed 1296 g. Notice the dramatic improvement in waist circumference with overall improvement in truncal outline, including hip and buttocks shape (Fig. 3).
Patient Examples From Dr. Nahas
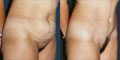
This 38-year-old woman presented with a Type III/A deformity, according to the classification described in 2001.2,3 For this type of deformity, the diastasis is corrected by plicating the anterior rectus sheath, and the excess skin is removed from the umbilicus to the inferior abdominal fold. She is shown preoperatively and 4 years postoperatively, demonstrating the long-term result of plicating the musculoaponeurotic layer (Fig. 4).
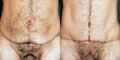
This 45-year-old man lost 40 kg and presented with a type II/B deformity. In addition to plicating the anterior rectus sheath, a vertical external oblique aponeurosis plication was also performed. Some of the skin of the lower abdomen was maintained, resulting in a small vertical scar. He is shown preoperatively and 8 months postoperatively, with a good abdominal contour in which the paramedian sulcus can be seen. This is the result of the external oblique plication (Fig. 5).
Reference
- Pollock H, Pollock T. Progressive tension sutures: a technique to reduce local complications in abdominoplasty. Plast Reconstr Surg 105:2583-2586, 2000.
- Nahas FX. An aesthetic classification of the abdomen based on the myoaponeurotic layer. Plast Reconstr Surg 108:1787-1795, 2001.
- Nahas FX. A pragmatic way to treat abdominal deformities based on skin and subcutaneous excess. Aesthetic Plast Surg 125:365-371, 2001.

